
English for Healthcare: from Expertise to Practice — Kraków, September 2026
News · Conference We are delighted to announce that Specialist Language Courses is a sponsor of English for Healthcare: from Expertise to Practice, an international

If you are preparing for the OET Medicine speaking sub-test, questions are not simply a device for gathering information — they are the backbone of the entire role play. Whether you are exploring a patient’s concerns, confirming what they already understand, or giving them space to express how they feel, almost everything you do in the role play is driven by the questions you ask.
This article explains exactly which questions to use, when to use them, and why they matter for your clinical communication criteria score. Read on to discover how asking the right questions — and avoiding the wrong ones — can make a real difference to your OET result.
In the OET speaking test you perform two role plays, each with a patient or carer. Across both role plays you are assessed on your ability to:
These are not separate tasks — they are deeply interconnected, and questions thread through all of them. Even when you are providing information, you need questions to check understanding and invite a response. The OET marking criteria make this explicit, which is why developing a reliable question-asking strategy is so important.
Questions serve six distinct purposes in the OET speaking role play. Understanding each one — and having ready-made language for each — gives you both flexibility and structure during the test.
Eliciting and exploring a patient’s ideas, concerns, and expectations is one of the specific items assessed under the clinical communication criteria. Despite this, it is one of the areas where candidates most commonly lose marks, because they focus entirely on symptoms and forget to ask how the patient feels about their situation.
Use questions such as:
“Do you have any idea what might be causing it?”
“Is there anything that concerns you about that?”
“What were you hoping we might be able to do today?”
The information-gathering criteria reward candidates who use a deliberate sequence of open and then closed questions. Start with an open question to let the patient describe their experience in their own words; follow up with closed questions only where you need specific details.
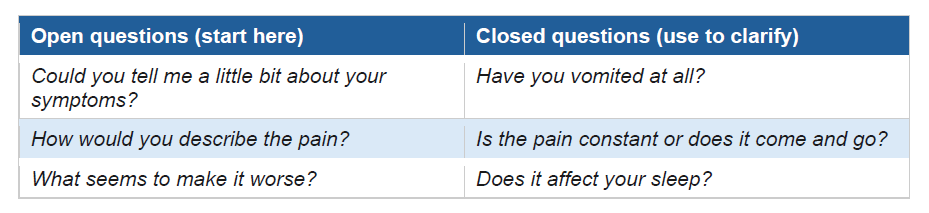
The same principle applies when exploring lifestyle. Rather than launching straight into advice, ask first:
“Could you tell me a bit about your diet?”
“How much exercise do you usually do?”
This allows you to tailor any advice to the patient’s actual situation rather than delivering generic information.
When a patient uses vague language, or when you need more detail about something they have said, clarifying questions show that you are listening carefully and that you want to understand accurately.
“What do you mean by feeling funny?”
“You said you felt off balance — do you mean dizzy?”
“You mentioned you often vomit after exercise. How often would that be, exactly?”
You can also use questions to summarise and check your understanding, or to invite the patient to add anything you may have missed:
“So you were cleaning the house, and then what happened?”
“You said it is worse after exercise but not bad at rest — is that right?”
Before you explain a condition or treatment, check what the patient already understands. This avoids repeating information they already have and helps you correct any misconceptions. It is also assessed under the information-giving criteria.
“Could you tell me what you know about asthma?”
“How much do you know about this condition at the moment?”
When providing information, it is not enough simply to deliver it — you need to pause at intervals, check whether the patient has understood, and give them an opportunity to respond. This technique is known as chunking and checking: you deliver a chunk of information and then check in with a question before moving on.
Useful checking questions include:
“Does that make sense so far?”
“Is that clear?”
“Do you have any questions about what I have just explained?”
To encourage the patient to say how they feel about the information:
“How do you feel about that?”
“How does that sound to you?”
Questions are also one of the most effective tools for managing the flow and structure of the conversation. You can use them to open the role play, to transition between topics, and to obtain consent before asking a series of questions.
Opening the role play:
“Could you tell me what brings you here today?”
Transitioning between topics:
“Would you mind if we talked about your lifestyle for a moment?”
“I’d like to explore the treatment options with you now — is that all right?”
Obtaining consent before a series of questions:
“I’d like to ask you some questions about the pain, if that’s OK.”
“Would you mind if I asked you a few questions about your lifestyle?”
These last two examples are particularly important: they demonstrate a respectful attitude toward the patient which is also part of the clinical communication criteria you are assessed on.
Not all questions are effective, and two types are specifically penalised under the information-gathering criteria.
Avoid these question types
The chunking and checking technique deserves a section of its own because it is frequently overlooked — and yet it directly relates to several parts ofthe OET criteria. Many candidates focus on delivering information and forget that communication is a two-way process. The patient needs to process what you are telling them, and they need the opportunity to ask questions or express doubts.
A simple framework to follow:
Step | What to do |
1 | Deliver a small chunk of information (two to three sentences maximum). |
2 | Pause. |
3 | Ask a checking question. |
4 | Allow the patient to respond before continuing. |
One of the marks of a confident OET candidate is the ability to manage the flow of the conversation naturally. Using questions at key transition points not only keeps the role play on track but also signals to the examiner that you are in control of the interaction without being directive or dismissive.
Think of the role play in three broad stages, and consider which questions fit each stage:
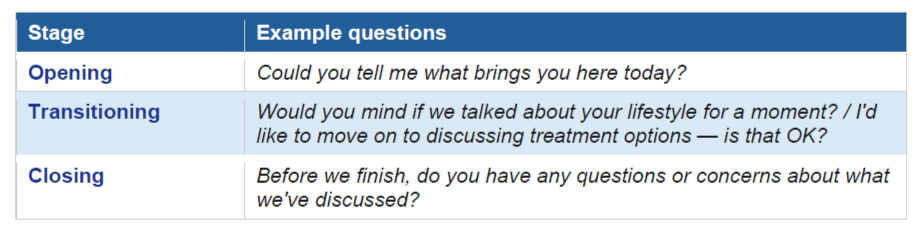
Before taking the test, practise using questions actively rather than passively. When you work through a role play card, go through it section by section and brainstorm the questions you might need at each point. Do not forget to include questions for checking understanding and inviting the patient to share their feelings.
For example, a role play card task might ask you to: explain recent test results, advise on lifestyle changes, and discuss next steps. Every one of those tasks will require questions, not just information delivery. You might need:
Working through role play cards systematically in this way helps you build a question bank that feels natural and automatic on test day.
Top tips for asking questions in the OET speaking test
Specialist Language Courses (SLC) are dedicated to helping healthcare professionals excel in the OET. Our expert-led courses focus on the specific language skills and test strategies needed to succeed. With personalised coaching, practice tests, and targeted exercises, we ensure you build the confidence and competence required for each OET sub-test. Join SLC to boost your chances of achieving the scores you need and advancing your healthcare career

News · Conference We are delighted to announce that Specialist Language Courses is a sponsor of English for Healthcare: from Expertise to Practice, an international
News · Institutional We are delighted to announce that Specialist Language Courses has launched a new institutional licence, giving university and college students access to

Back to Menu ↩ In the OET Speaking sub-test, you perform two role plays in which you are assessed on your ability to ask questions,
Get updates and get the latest materials on Medical English, OET and IELTS
15% OFF all 1-month & 3-month course subscriptions!
